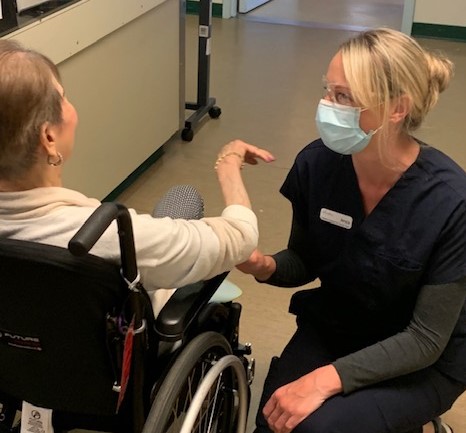
When Jenica Burns and Kelly Konyk joined the nursing staff at four long-term care sites during the height of their Covid-19 outbreaks last year, the nurses appeared as a bright spot in a dark time.
The two members of the Providence Health Care’s Palliative Outreach and Consult Team (POCT) had been seconded to various sites across the Lower Mainland to help staff meet the complex needs of vulnerable residents stricken by the virus.
Working with COVID-19 patients highlights “why I work in palliative care”
That experience resonates deeply today. “I’ve always believed in palliative care, and that’s why I went into nursing,” says Konyk, who currently works at Providence’s St. John Hospice. “After working in a pandemic with patients with Covid-19, it highlighted even more why I work in palliative care.”
With National Hospice Palliative Care Week May 2 – 8 underway, Konyk and Burns reflect on how broad palliative care is—even as the practice is dogged by myths and public assumptions that elicit fear and confusion among the public and do a disservice to families, patients and caregivers.
Palliative care doesn’t mean the end
Often when people hear their family member will be receiving palliative support in a long-term care setting, they assume that their loved one is at the end of their life, but that’s not always so. A palliative approach to care should start early, at the time of diagnosis with a life limiting illness. During several COVID outbreaks, Jenica and Kelly were able to provide education for staff, mobilize resources, support families and help alleviate symptoms for residents ill with COVID, the majority of whom recovered from the virus.
“We’re constantly challenging this idea that palliative care is specifically for those who are dying,” says Burns, who has been part of the POCT team and worked in long term care throughout Providence since 2010. She’s currently based at St. Vincent’s: Brock Fahrni and Holy Family Hospital.
“I value those sacred moments where I can sit and be present with someone while they’re dying, but it’s a lot more than that,” adds Konyk. “The constant soothing and handholding is a myth. It can be quite intense work.”
Simply put, palliative care focuses on managing pain, treating symptoms and building relationships with patients and families. POCT team members use all their expertise to provide symptom relief associated with chronic diseases such as heart failure, cancer, respiratory disorders, renal failure, degenerative neurological diseases or infections from illnesses.
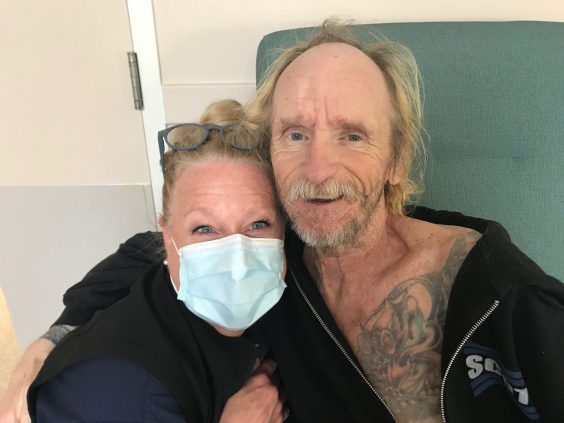
“My experience has been that once residents and families see how palliative care can be woven into the fabric of their overall care, there’s more acceptance, less fear and people are often very grateful for the care provided,” says Burns.
Empowering Patients and Families from the Beginning
Once patients and families understand palliative care doesn’t always equate to end-of-life care, they know enough to dismiss another myth: that treatment is all about following health care providers’ orders, while patients and families remain passive during the course of the illness.
The nurses stress that when the palliative team is involved soon after a palliative diagnosis, the collaboration allows a patient to create their own road map of their futures. If it’s early and proactive, the goal setting provides an energy that improves their quality of life.
That work tracks with renowned research that shows a palliative approach to care, begun early in the trajectory of a life-limiting illness, reduces the length of patients’ stay and a number of in-hospital deaths.
Patients and residents should be involved in decision making about their health, says Burns, “this is a fluid process, and it’s about understanding what is most important to them. Communicating their wishes gives us as a team a good understanding of their goals.”
Palliative care not black or white
The nurses’ experience with Covid-19 patients illustrates points brought forward in studies that dispel another popular myth: you’re in the hospital to be treated and begin to recover or you’re in palliative care and preparing for end of life.
“It’s not black or white. You can receive a palliative approach to care while receiving treatment. Those two things should be woven together,” says Burns.
In fact, palliative care is an essential part of a collaborative approach and often accompanies the work of physicians, social workers, occupational therapists and physiotherapists, pharmacists, and dieticians.
Ultimately, as a palliative approach is integrated into every facet of health care, these public myths will likely fade from public imagination—and “that’s gradually happening within Providence Health Care,” says Burns.
“We’re building capacity within the care teams we’ve worked with, and that has gone a long way to provide ongoing education that will de-mystify palliative care,” says Burns.