It’s called ‘liquid gold’, and for good reason. After a small sip of colostrum – the thick, amber breast milk secreted in late-stage pregnancy and immediately after birth – a newborn baby gets the instant dose of nutrition, antibodies and antioxidants it needs for a boost of immunity and a healthy first few days of life.
Now, thanks to an initiative inspired from a nation-wide Baby-Friendly Initiative (BFI) quality improvement project, more patients at St. Paul’s Primary Care, Maternity Care Clinic are breastfeeding and providing colostrum to their newborns. It’s an apt project for World Breastfeeding Week, a global campaign to raise awareness of the benefits and importance of breastfeeding.
Interdisciplinary approach brings project to life
“This project is very much a team effort,” says Amy Hamill, the Patient Care Manager for Maternity and NICU at St. Paul’s. “It is a true interdisciplinary approach across Maternity and NICU and very much nurse-led.”
St. Paul’s Hospital Clinical Nurse Educator Andrea Firmani says that when she began as a maternity nurse nearly 18 years ago, patients were encouraged to breastfeed but may have found it difficult to find support.
“About 99 per cent of people came in to us and said their plan was to breastfeed. And we’d tell them, ‘that’s great, we’ll see how it goes,’ but we didn’t really have a lot of supports in place to help people meet their goals.”
Prenatal support landscape in BC vastly improved
Since then, the landscape of birth support, prenatal care and education surrounding breastfeeding in BC has transformed. New and expectant parents are more active, confident and empowered to make choices that determine their health and that of their newborns before and after birth.
Through the Baby-Friendly Initiative, they explored patients’ experience from pregnancy through to birth, but Firmani says that from surveys and patient charts, they noticed that patients who wanted to breastfeed exclusively were not doing so.
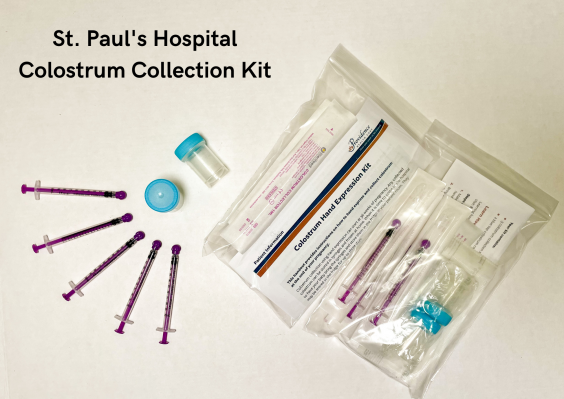
Today, many St. Paul’s maternity patients receive a colostrum collection kit during pregnancy, equipping them with the information and gear to collect this nutrient-dense colostrum in anticipation of feeding the new baby directly after birth.
Big jump in discharged moms exclusively breastfeeding
The project set the stage for a pilot study in 2021 that would eventually give them an even greater sense of control and confidence. In the end, the project changed patients’ lives.
In the first part of the project, about 50 per cent of patients left the hospital exclusively breastfeeding. That figure has risen to 80 per cent.
“We changed our level of support, whether that is prenatal education, the colostrum collection kit, access to staff trained in breastfeeding,” Firmani says.
From Idea to Pilot Project to a First in BC
It all began when Dr. Evelyne Perron, a co-lead physician with Dr. Jennifer Leavitt at the Primary Care and Maternity Care Clinic, attended a conference in eastern Canada in September 2021. There, discussion turned to the benefits of colostrum collection, and another physician’s experience with coaching expectant parents to hand- express it during pregnancy. Hand expressing refers to a gentle massage of the breast to stimulate milk receptors.
Inspired, Dr. Perron floated the idea to the BFI Leadership team, including Firmani, who worked with her to pull together a list of criteria and gather a control population for a study among patients at or after their (36th week) of pregnancy.
They then compiled Colostrum Collection Kits, including a syringe and instructions on how to express what they hoped would be even the smallest drop of colostrum, in anticipation of a newborn’s first feed.
Participants were asked to try to collect colostrum through hand expressing, or gently massaging the breast to help stimulate milk receptors and catch a drop on the nipple.
After coaching and practice, those patients who produced colostrum stored it in their home freezer before it went to the refrigerator in their St. Paul’s birthing room. There, the colostrum was warmed and fed to babies by spoon or syringe. The quick timeline from there meant no big gaps between birth and colostrum feeding.
Success is in the Learning Process
Participants were surveyed postpartum.
The reactions were encouraging, no matter how much colostrum was produced, whether a few drops, or nothing. The most common feedback from patients was their increased confidence in the final stage of pregnancy.

In an effort to normalize that collecting colostrum, and breastfeeding in general, can be challenging for some, the maternity unit provides support with a breastfeeding clinic, a lactation consultant and a postpartum support group.
“Breastfeeding can be very challenging for some people. And it’s associated with feelings of not being ‘enough’,” says Dr. Jennifer Leavitt. (Dr. Perron is now on maternity leave).
At St. Paul’s, kits are available in the family practice maternity clinic and some midwife and OB offices; fetal monitoring patients and anyone who attends in-person pre-natal classes can access them as well.
Even just the process of learning of the benefits of colostrum during prenatal visits encourages more conversations about breastfeeding between clinic staff and patients, Dr. Leavitt adds.
“These conversations can empower patients on their breastfeeding journey before it even starts. It feels motivating to have something you can do, that’s in your control.”





