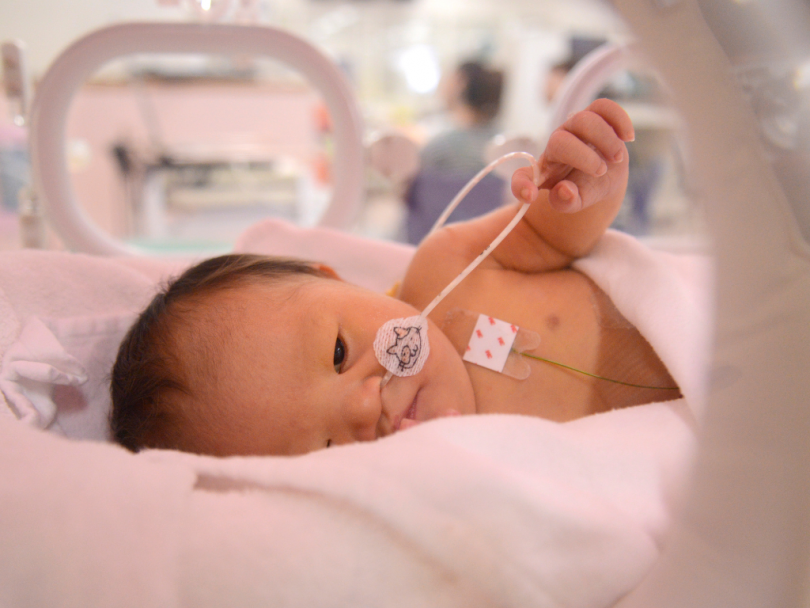
The biggest transformation in care is in store for the smallest patients St. Paul’s Hospital will treat at its future site.
The new Neonatal Intensive Care Unit (NICU) is one of the best examples of how care will be transformed at the new St. Paul’s Hospital.
Family-centred model guides design
“The new NICU is going to be completely different for families,” says Emily Welsh, a Providence Health Care NICU and Maternity nurse. “We’ll be using a ‘family-centred’ model of care which will change almost everything.”
Currently, NICU uses a ‘nursery-style’ model of care where up to eight families share one large communal room that also includes the care team station. Each family and its incubator are confined to their portion of the room. Some families benefit from the shared experience and camaraderie of this communal setting. But others would appreciate more privacy as they’re going through this tough time, and less exposure to the anxiety of others.
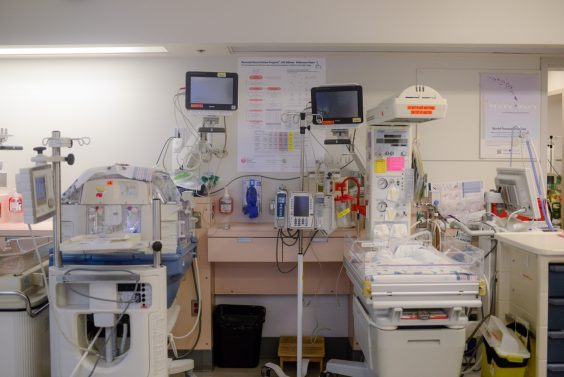
Currently, until they’re discharged, all NICU birth parents stay in rooms down the hall in the Pregnancy, Birthing and Newborn Centre and walk or wheel over to the NICU to see their little one, which can be challenging for some parents who have postpartum complications. And, any baby born here before 32 weeks of pregnancy is transferred to BC Women’s Hospital (which cares for the most premature babies in BC), while the parent stays behind at the hospital, and that can be tough for families.
“Meeting baby’s needs has always been a priority for our team, but our new NICU will reinvent the family’s experience,” says Welsh, who has been a Providence NICU nurse for over six years.
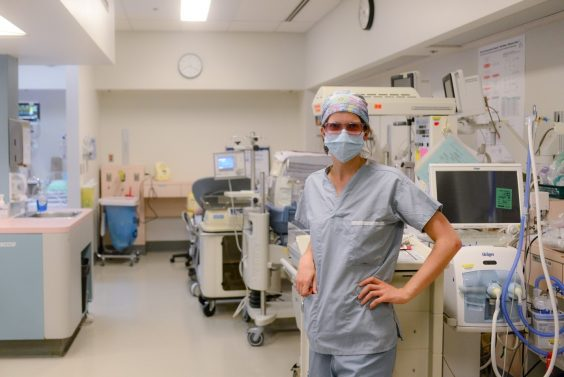
New NICU to be better in three big ways
Welsh says the NICU on the second floor of the new hospital will see three important improvements:
“First, instead of a communal nursery, each family will have their own room and washroom, plus a comfy sofa bed so family can stay at their baby’s bedside all day, every day, if that’s what they want. The goal is to create a much more relaxed, comfortable and private environment for every family.
“Second, we’ll be able to care for low-risk postpartum parents inside the NICU rooms. Each NICU room is big enough for an incubator….and a maternity bed.
“And third, we’re planning to care for sicker babies — born at 30 weeks or later, versus 32 weeks.” This two-week difference represents a lot of the babies St. Paul’s transfers today to BC Women’s Hospital. Transitioning the NICU to this higher level of care means more birth parents and babies can stay together rather than being cared for in separate hospitals.”
Full-sized NICU floorplan helps staff give input into design
Members of the NICU team toured a full-scale NICU room floorplan to give input on the layout of two rooms.
This paper mock-up exercise tested if a maternity bed could fit inside the two NICU rooms that accommodate two incubators each, for twins. Could the maternity bed be easily moved in and out of the room if the birth parent suddenly needed to go to the maternity operating room? It’s part of why Craig Harris, a senior project and change management lead for the New St. Paul’s Hospital and Health Campus Project, thought a paper mock-up test drive of this particular NICU patient room might help. The answer was yes, the bed fits.
“We want parents to feel like their needs are being met alongside their baby’s, and that we’re treating them as a whole family unit,” says Harris.
Staff involvement in the design process also means a laundry room has now been added – a priority for some families who can spend months here.
Wireless tech to connect staff in emergencies
Single-family patient rooms will result in some changes for how staff work.
“We’ll likely have wireless communication devices so staff can connect with each other in emergencies. Today, when we’re in our communal nursery our team can just talk to each other from across the room and we have eyes on all our babies and all the vital sign monitors,” explains Welsh. “Single-patient rooms will change that. But technology will help.”

To learn more about the project and engagement for the new St. Paul’s Hospital, visit its website.