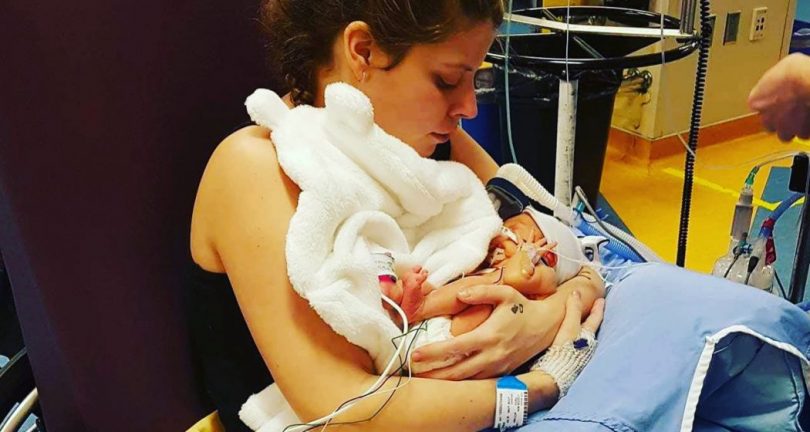
Jaxon Gallagher is almost two and that’s something of a miracle.
The little boy was born prematurely at St. Paul’s Hospital in April 2017, weighing just three pounds, 11 ounces.
His mother Brittany had gone into cardiac arrest at the hospital when she was seven months pregnant. Multiple care teams gathered with lightning speed to revive Brittany and deliver Jaxon by emergency C-section.
Both have made full recoveries.

It was the most dramatic case Brittany’s caregivers had ever seen, and one that Dr. Judy Wolfe, Site Head for Pediatrics at Providence Health Care, is reminded of this World Prematurity Day.
World Prematurity Day
It’s celebrated globally on November 17 to bring awareness around premature birth, the main cause of death in children under age five, according to the World Health Organization. Premature birth can lead to long-term health issues affecting the brain, lungs and sight.

Caring for pregnant moms who have such severe health issues or injuries they risk delivering preemies (defined as 37 weeks or less at birth compared to the full term 40 weeks for singletons) is not always as dramatic as Brittany’s case but it’s standard at St. Paul’s, Dr. Wolfe says.
St. Paul’s cares for sick moms with complex-care needs
The hospital is the provincial centre for high-risk maternal care. About a fifth of all babies born there are to mothers with complex-care needs. Moms may have organ-transplant issues or substance-use problems or – like Brittany – cardiac problems. And they’re more likely to have tiny babies.
St. Paul’s works closely with BC Women’s and Children’s Hospital. “BC Women’s takes care of sick babies and healthy moms. St. Paul’s takes care of sick moms. The excellence is there in so many of our programs.” Young Jaxon was transferred to BC Children’s immediately after he was stabilized.

Providence’s patient- and family-centred care has helped St. Paul’s make advances in preterm care overall. In the new year, it will take part in a provincial “Kangaroo Care” Skin to Skin program, providing wraps to family members of the preterm babies to encourage longer, more comfortable periods of hands-free skin-to-skin time.
“We do not see the infant as our only concern,” says Anna Paraninfi, clinical nurse educator at St. Paul’s Nenonatal Intensive Care Unit (NICU). “We’re there to support the parents and have them as equal partners in their baby’s care.”
This is a newer approach to caring for preterm infants, says Ms. Paraninfi. “In prior years, the nurses would provide direct care. But we have come a long way in teaching families to become the care providers for their babies.”
Dr. Wolfe says that, in general, keeping mom and preemie together stabilizes these tiny babies, even those who are born as early as 25 weeks. Moms with health problems who have been stabilized, including psychiatric issues or substance-use disorder, are encouraged to keep their babies together for the well-being of both.

St. Paul’s has also improved the feeding of preterm babies through the years. It uses donor breast milk from BC Women’s for moms with other medical problems who often have delayed milk production.
Preemies, particularly those born at 32 weeks or less, are at risk for a serious and often deadly intestinal condition called necrotizing enterocolitis, says Dr. Wolfe, but research has found that breast milk can markedly decrease the risk of the preterm infant contracting or dying from it.
Outcomes improving
Dr. Wolfe says that because of the comprehensive medical care for the mom and the maternal care for the preemie, the hospital is seeing better outcomes for these tiny infants. “Even 24 to 25-week old babies are likely to survive. Once they get to 28 weeks, the survival rate increases to over 90 per cent. And at 32 weeks, it rises to more than 96 per cent.”
She is proud of the hospital’s care for the high-risk moms across the province who may be at risk of delivering preterm babies.
“We take all comers.”
Read more about Brittany and Jaxon here.