When the pandemic hit back in March 2020, most research activities at Providence Health Care and other institutions around the world were curtailed, with the exception of COVID-19 studies. Almost overnight, many researchers dropped their work and pivoted all their attention to SARS-CoV-2.
The year 2021 saw a gradual re-opening of research at Providence, but many investigators continued to focus their efforts on COVID-19. They collectively secured millions of dollars in COVID research funding and harnessed existing equipment and expertise to launch dozens of COVID-related studies – from diagnostic research to interventional clinical studies and community research.
As we prepare to usher in 2022, we’re looking back on the year that was and some of the biggest COVID-19 research news involving Providence Health Care.
In no particular order, and by no means a comprehensive list, here are 10 COVID-19 PHC research highlights from 2021:
COVID-19 vaccine uptake, side effects in at-risk groups
Research by the BC Centre on Substance Use at St. Paul’s Hospital and other groups received $770,000 to investigate the uptake, effectiveness and side effects of COVID-19 vaccines among vulnerable urban populations.
The people included experience risk factors such as homelessness and poverty. Adding to these risks are the barriers to vaccination, ranging from stigma to discrimination, which they already often face when trying to access health care.
This research will support the development of more effective vaccination and public health strategies to reach those who are most vulnerable to harms and severe outcomes from COVID-19 in urban areas.
Solving the puzzle of COVID-19’s long-term impact
Why do some people infected with the virus that causes COVID-19 get severe disease while others have no symptoms? Why do some experience long-term effects and others recover quickly?
A research study hopes to answer these questions. The study is part of the Canadian COVID-19 Prospective Cohort Study (CANCOV), a cross-Canada effort that will pool data from sites in six provinces, including St. Paul’s Hospital.
Led by Dr. Anita Palepu, the B.C. arm aims to enrol 500 people. Participants will be followed for up to three years after their initial infection, making this the first study in Canada to explore long-term outcomes of patients across the spectrum of COVID-19 severity.
Weaker antibody response to first COVID-19 vaccine dose found in long-term care residents
A single dose of the Pfizer-BioNTech COVID-19 vaccine produces a much weaker antibody response in long-term care residents than it does in younger healthy adults, research found.
Medical leader for medical microbiology and virology at St. Paul’s Hospital, Dr. Marc Romney, and the research team, co-led by Dr. Zabrina Brumme of the BC Centre for Excellence in HIV/AIDS and Dr. Mark Brockman of SFU, analyzed blood samples collected in late 2020 and early 2021 from residents and staff of long-term care homes in Metro Vancouver.
Their findings raised questions about the optimal timing of the second dose of vaccine for older adults.
Pan-Canadian study assessing COVID-19 vaccine response in those with HIV
People living with HIV are less likely to mount an adequate immune response, which may put them at higher risk for both serious COVID-19 illness and reduced response to COVID-19 vaccination. Now, a $2.6 million study is assessing the immune responses, safety, and effectiveness of COVID-19 vaccination for people living with HIV.
Conducted by the CTN (housed at St. Paul’s Hospital), and a large team from across Canada, the study, called COVAXHIV, is the most extensive study in Canada to date to evaluate the immunogenicity, safety and effectiveness of COVID-19 vaccination in a diverse population of people living with HIV.
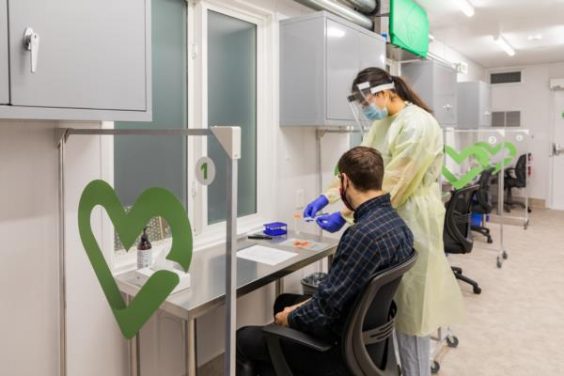
WestJet-YVR COVID-19 study shows rapid antigen testing is effective in screening travellers
The Vancouver Airport Authority and WestJet released study findings in April showing that rapid antigen testing is an effective, acceptable and cost-efficient method for screening travellers and contributes to safer and healthier air travel.
Over four months, nearly 600 departing passengers at YVR were tested for COVID-19 using rapid antigen testing. All tests administered during this period were negative.
Researchers from UBC and Providence were responsible for collecting samples in a ready-made testing station. Results gathered were further validated through PCR testing in a lab environment.

Stronger immune response from delaying second dose of COVID-19 vaccine
The first peer-reviewed study in North America examining dosing intervals for COVID-19 mRNA vaccines showed a delayed second dose leads to a stronger immune response. Principal investigator Dr. Brian Grunau says these results could inform ongoing international COVID-19 vaccination efforts.
Researchers compared blood test results from paramedics who were vaccinated within the interval of less than four weeks, to those who received their second dose after six to seven weeks. Participants are enrolled in the larger national study examining how the pandemic has impacted paramedics.
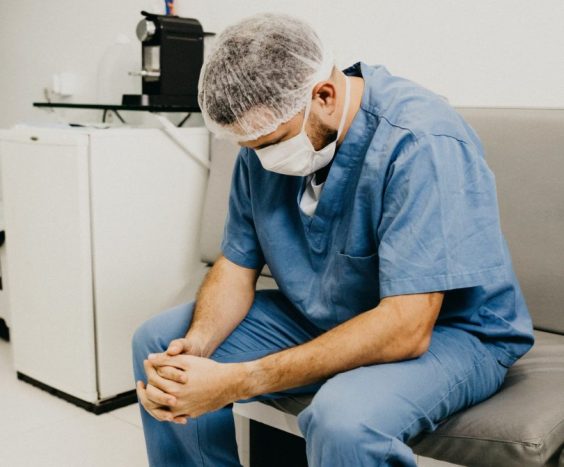
Pandemic shows need to address physician burnout
A research team led Dr. Nadia Khan, a UBC general internal medicine professor and St. Paul’s Hospital physician, reviewed survey responses from 302 internal medicine physicians who worked for Vancouver General Hospital and St. Paul’s Hospital between August and October 2020.
They found burnout was prevalent among 68 per cent of physicians and noted over 20 percent of surveyed physicians were considering quitting the profession, or had already quit a position.
The findings highlight the need to focus more on the mental health and working conditions of doctors, nurses, and other healthcare workers.

COVID-19’s impact on people with opioid use disorder
People who use drugs may be more likely to contract COVID-19 and, if they do, experience more severe illness and poorer outcomes due to underlying medical conditions. People with opioid use disorder have an even higher risk of contracting COVID-19 than people with other substance use disorders.
A study involving several Providence researchers sought to understand the experiences and needs of people with opioid use disorder during the pandemic. The team focused on people who were not already receiving opioid agonist therapy to get the perspectives of those at greatest risk for overdose and death.
Participant interviews revealed that COVID-19 had a significant impact on how people used drugs and peoples’ feelings toward helping others.

No increase in suicide in the early days of COVID pandemic
A publication showed that suicide rates in B.C. did not increase in the first phase of the COVID-19 pandemic, counter to earlier predictions made by some experts and commentators.
The research team compared provincial suicide rates in the first phase of the COVID-19 pandemic (March to August 2020) to rates in the previous 10 years.
“We did not observe an increase in suicides during this period. If anything, we saw a slight decrease,” said research lead Dr. David Barbic, an emergency physician at St. Paul’s Hospital and a clinical assistant professor at the UBC Department of Emergency Medicine.

COVID-19, structural racism and migrant health in Canada
A paper published in The Lancet by researchers with the Centre for Gender and Sexual Health Equity calls for urgent action on structural racism amidst the global pandemic.
The paper explores the disproportionate impact of COVID-19 among racialized migrants in Canada, a high-income migration destination country. It acknowledges structural racism as key to understanding health inequities faced by racialized migrants, noting that migrants are overrepresented in essential jobs yet face unequal access to health and other support services.
The evidence calls for urgent action in order to meet the human rights needs of racialized migrants.