September is the awareness month for a type of cancer that gets little attention, but is rising in cases every year – thyroid cancer.
“It’s a cancer type that most people haven’t heard much about, but that is becoming more commonly diagnosed,” says Dr. Sam Wiseman, a thyroid surgeon and researcher at St. Paul’s Hospital.
More common in women than men
Cancer of the thyroid, the butterfly-shaped gland at the front of your neck, is projected to be the 13th most common cancer diagnosed in Canada in 2022. Some 6700 new cases will be diagnosed this year. The majority of these cases, 72 per cent, will be diagnosed in women, for reasons that are not well understood. The diagnosis rate of thyroid cancer has been steadily rising in Canada and around the world for longer than 30 years.
Rise in cases due to better diagnostics
But don’t panic: thyroid cancer is very treatable. When properly managed, it has excellent outcomes for most people. The rise in cases has been largely attributed to the widespread availability and usage of diagnostic imaging tests, especially neck ultrasounds, and it has not been accompanied by a similar rise in thyroid cancer-related mortality rates.
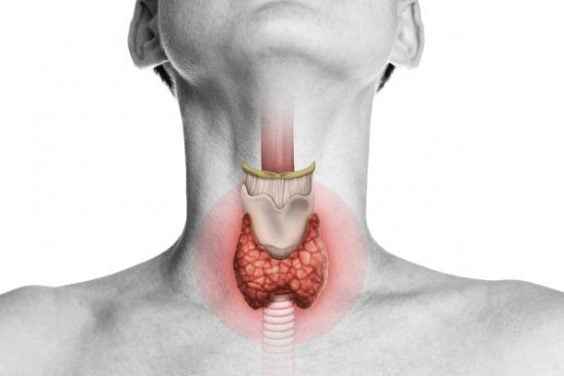
In general, says Dr. Wiseman, the vast majority of people diagnosed with thyroid cancer have an excellent outlook. Their lifespan is not shortened. However, it is important to be aware of the signs and symptoms of this cancer type. Talk to your doctor if you notice a lump on your neck. Though the vast majority of neck lumps are not cancerous, it’s very important for you to be checked out by your doctor if you notice one.
What should you look out for?
The majority of thyroid cancer cases are not symptomatic. In 2015, Dr. Wiseman published a study reporting on a group of patients with the most common type of thyroid cancer, papillary thyroid carcinoma, who had tumors larger than one centimeter. In 53 per cent of cases, the thyroid cancer was found incidentally either during imaging being carried out for other reasons, or during an examination by a physician. People with thyroid cancer may also have symptoms that include a change in their voice or difficulty swallowing or breathing, but these are uncommon.
“Really, what people need to look out for is a lump in their neck,” says Dr. Wiseman.
What makes someone higher risk for thyroid cancer?
Certain factors increase a person’s risk of developing thyroid cancer, such as a history of the disease in multiple family members, or a history of radiation exposure, particularly of the neck. Thyroid radiation exposure may have happened as part of past treatment of other cancer, especially if it occurred during childhood.

Apart from your physician examining your neck during a physical check-up, thyroid cancer is not routinely screened for unless you have one of these risk factors. While some thyroid nodules may be cancerous, 95 per cent are benign.
An advancing field
The ways in which thyroid cancer is investigated and treated has evolved significantly over the past several decades, becoming more consistent and evidence-based. Improved consistency in thyroid ultrasound reporting, with the adoption of a standardized system for describing the appearance of the thyroid gland and its nodules, has enabled doctors to determine which nodules warrant a close follow-up, and which need to be biopsied. This has led to a reduction in the number of procedures performed for what is eventually found to be a benign disease.
Other innovations in thyroid cancer management include the implementation of a standardized system for reporting the results of needle biopsies, and an evolution of treatment guidelines that allow for more tailored surgical management – for instance, some patients only need half of their thyroid removed.
Research still being done to further improve patient outcomes
Much of Dr. Wiseman’s research focuses on improving the quality of care and outcomes of thyroid cancer patients. One current project he is working on, in collaboration with a panel of thyroid surgery experts from across Canada, is to develop a standardized synoptic operative report for thyroid surgery.
Surgeons create operative reports after a procedure is completed in order to communicate important details of the surgery to the healthcare team involved in the patient’s care, which can influence additional treatment and follow-up. The standardized synoptic operative report that Dr. Wiseman and his team have developed, which is currently being studied, would ensure specific information is included to improve the consistency and quality of patient care and potentially lead to better outcomes.
It’s not only important to be informed about what factors increase your risk of developing thyroid cancer and the signs you should look out for, but also to be aware of the advancements in the field and the research that continues to be carried out, here in BC and beyond.
Ultimately, it aims to improve the lives of people diagnosed with this common cancer type.