It’s Digital Health Week November 29-December 5, an annual week to recognize how digital technology is transforming health care in Canada.
IPads secured by Providence Health Care during COVID-19 are offering comfort to families with loved ones who are at the end of their lives.
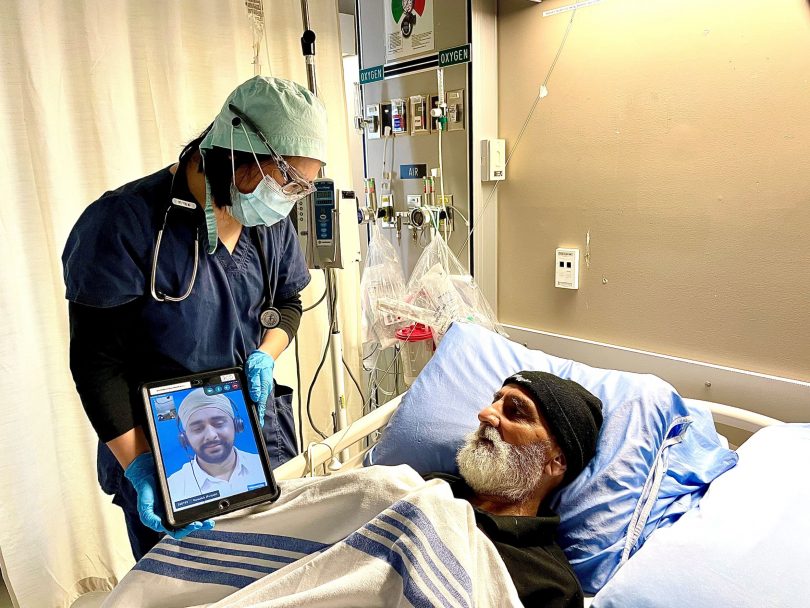
The tablets, obtained when COVID-19 forced hospital visits to be restricted, feature a video interpreter app to help patients and families communicate with the care team when not all the parties understand English.
Closure at emotional times
It virtually unites dying patients with family members who can’t visit in person, and lets everyone see one another.
The interpreter function provides closure in an emotional time, says Hecel Peakman, Clinical Nurse Leader at St. Paul’s Cardiac Surgery ICU.
That was the case for a Vietnamese-speaking family recently, she says.
They lived in the BC Interior and were unable to get to St. Paul’s Hospital to say final good-byes to their loved one. The video interpreter explained all the details of the situation in Vietnamese. “The family could sing their songs and say their good-byes over video,” says Peakman. “The family’s ability to meet in this way with the health care team helped tie everything together.”
Patient’s doctor spoke to relatives in Brazil
In another recent case, the doctor of a patient with relatives in Brazil used the app so a Portuguese-speaking interpreter could fill them in on the loved one’s condition and care plan.
The app is another way digital health has helped health organizations adapt to COVID-19 to continue to give patient-centred and compassionate care.
It opens with a single click. A search field appears so the user can type in the desired language or use a drop-down menu.
Another click, then the interpreter appears on the iPad and the communication begins.
“It’s in real time,” explains Celeste Cardoz, Virtual Health Specialist at Providence Health Care.
“You see the interpreter’s face and the body language. That helps the patient see the interpreter, making it less disorienting than speaking by phone.”
Virtual tool lends humanity to family-health care team interactions
The professional interpreters the app provides (via a third party service called LanguageLine Solutions) are medically trained to provide accurate translations of medical concepts and vocabulary a family member might not know.
For end-of-life patients, there is a sense of comfort in being able to see someone instead of hearing only a voice. It lends humanity to the interactions with family and health care providers at a sad, intense time.
What’s more, because it reduces the logistics around finding in-person interpreters, which was the approach pre-COVID, it permits care teams to make decisions more quickly.
“The virtual interpreter app is an effective way to increase accessibility, while maintaining the quality of interpreting service, and being cost-efficient,” says Margot Wilson Director, Shared Care & Virtual Health at Providence.
The app on the 87 tablets Providence purchased for COVID use is helping throughout the organization.
Because there is an American Sign Language interpreter option, it can help in situations involving hard-of-hearing patients.
Virtual interpreter has uses across Providence
It is also important in long-term care for residents with dementia who might be confused by talking to a faceless voice on a phone call.
It is helping clinicians in other units strengthen relationships with their patients and help them get well.
That has been the experience of Dr. Tina Lai, a family doctor who is a physician with Geriatric Medicine and the Complex Reactivation Unit at St. Paul’s. It cares for medically complex patients needing long hospital stays.
She used the virtual interpreter to translate for a Russian-speaking patient. “I developed an excellent relationship with the patient because without the interpreter, she felt no one understood her and could help her.”
“Language should never be a barrier to providing or receiving care.”